The Therapeutic Goods Administration (TGA), as part of the Australian Government Department of Health, was established in 1989 and protects the health and wellbeing of the community by regulating and monitoring all therapeutic goods that are distributed here in Australia.
Role of the TGA
TGA administers the Therapeutic Goods Act 1989 (The Act) - the same Act under which it was established. It maintains the Australian Register of Therapeutic Goods (ARTG) and plays an instrumental role in the Australian Government's implementation of the National Medicines Policy.
TGA regulates and monitors therapeutic goods by:
- authorising the commercial supply of therapeutic goods for use in Australia through the ARTG (an electronic register of therapeutic goods that can be lawfully supplied in Australia)
- monitoring the safety of therapeutic goods using information from various sources (the community, healthcare providers, overseas regulators and ARTG entry holders (sponsors) and manufacturers as a part of their reporting obligations)
- authorising manufacturers to ensure that products are manufactured to an appropriate standard
TGA is required to recover its costs through fees and charges for all activities that fall within the scope of the Therapeutic Goods Act 1989 including the TGA's public health responsibilities.
Importance of regulation
The need for regulation that would protect citizens against possibly harmful drugs, potions and devices is not new - in fact, it is older than Australia itself.
In colonial days there was legislation imposing controls on poisons, regulating pharmacists and attempting to limit some of the more outrageous claims made for patented medicines. These initiatives indicate an early recognition that the provision of medicines and other therapeutic goods could not continue in an unregulated climate.
The years after Federation saw a gradual accumulation of initiatives to meet the growing complexity of medical science. Examples of the steady flow of legislation that led to the emergence of the TGA in August 1989:
- the establishment of the precursor to the Commonwealth Serum Laboratories in 1915
- the passing of the Therapeutic Substances Act in 1937
- the provision of particular "life-saving and disease-preventing drugs" free of charge to pensioners in 1950
Australians have continued to take an interest in what the TGA does and the way it does it. Governments have responded to this, reflecting the cares and concerns of the people who have elected them.
Today, most major news outlets have their own dedicated health or medical reporter. In doing so, they are simply reflecting Australians' interest in and 'thirst' for health-related news.
Risk-based approach to regulation
The use of all therapeutic goods carries risk. When a bandage is applied to a minor cut that risk is negligible; the treatment of a headache with an everyday over the counter medicine carries more risk, but it is still small. The risk can be greater for a prescribed course of treatment for a serious illness. However, Australians have a right to expect that in all cases the medicines they take and the medical devices they use meet an acceptable level of safety and quality.
One of the roles of the TGA is to regulate therapeutic products based on an assessment of the evidence of the risks compared to the benefits of the therapeutic products. The TGA does this by applying scientific and clinical expertise. For more information, see Product regulation according to risk.
So that good decisions are made, the TGA employs Medical Officers who hold Australian Health Practitioner Regulation Agency registration, scientists, pharmacists and other highly qualified and experienced staff. The TGA also has access to independent expert advice via a number of advisory committees, which provides the TGA with access to Australia's most eminent and respected clinical and scientific experts.
As an example of how the TGA manages risks associated with the use of therapeutic goods, some medications for blood pressure may include side effects such as a tickle in the throat or a persistent cough. However, the risk of these irritating but minor problems is balanced against the possibility of a life-threatening heart attack if the medication is not used.
In other words, the TGA does not seek to avoid all risks - that would be impossible - but its risk management approach is about reducing the impact of risk to an acceptable level.
The amount of regulatory control needed to manage risks depends on the product and determines how consumers gain access to the product. A low-risk product may be safely sold in a supermarket; high risk products may only be supplied by prescription after consultation with a health professional.
The TGA also works to ensure that Australian and international manufacturers operate in a way that results in their products meeting required standards. It conducts regular inspections of manufacturers, both in Australia and overseas, to ensure they continue to meet these standards.
Two types of risk
The risks involved with therapeutic goods can be divided into two types:
- Product risks
- These risks are inherent to the product. They also include the risks involved in overdose (i.e. patient non-compliance)
- Compliance risks
- These risks are related to the risks involved if a manufacturer or sponsor fails to comply with legal requirements (either unintentionally or intentionally)
TGA actively regulates both product risks and compliance risks.
Product risk: pre-market activities
TGA regulates therapeutic goods before the products reach the market (pre-market) and afterwards, when they are in general use (post-market).
At the pre-market stage, TGA acquires the information necessary for a decision about whether or not to register, list or include therapeutic goods on the ARTG. We do this through accepting certification, actively evaluating information supplied by sponsors or manufacturers, or by direct inspection.
Medicines containing low-risk ingredients, including most complementary medicines, receive a lesser degree of checking than higher risk products, and are listed (AUST L) on the ARTG. The listing process is based on the certification of claims by sponsors. For products containing low-risk ingredients, regulation centres on the safety of the product and the consistency of the manufacturing process; less emphasis is placed on assessing the evidence for the claims being made.
Products carrying a higher risk, which include all prescription medicines, receive a higher degree of scrutiny and, if found to comply, are registered (AUST R) on the ARTG. Registration involves the evaluation of data related to safety, manufacturing and efficacy. Thus, when taking a therapeutic good that is registered on the ARTG, Australians can be confident that the product does not only meet safety and quality criteria, but that it has been demonstrated to have the claimed effect.
A similar risk-based approach is taken with the evaluation of evidence related to medical devices included on the ARTG. Low-risk devices (such as bandages) rely on certification, whereas high-risk devices (such as pace makers) involve direct evaluation of the available evidence by TGA.
Product risk: post-market activities
Post-market activities relate to the monitoring of the continuing safety, quality and efficacy of listed, registered and included therapeutic goods once they are on the market.
TGA has a strong pharmacovigilance program, which involves the assessment of adverse events that are reported to TGA by consumers, health professionals, the pharmaceutical industry, international medicines regulators or by the medical and scientific experts on TGA advisory committees.
Where a new risk is identified by TGA post-market activities, the best course of action is assessed. This may consist of adding a warning statement to the Product Information or recalling the product from the market.
Compliance risk: achieving voluntary compliance
It has been shown that a government regulator such as the TGA can achieve high levels of voluntary compliance through effective engagement and supply of information to those that it seeks to regulate (the regulated entities). Some of the key principles that underpin this 'responsive regulation' approach are:
- 'Benefit of the doubt' principle
- The assumption is that the majority of regulated entities intend to comply with the regulatory schemes
- Targeting likely areas of non-compliance
- It is important to identify individuals or sectors of the regulated community at risk of non-compliance by assessing risks and analysing data, and to take appropriate preventive action (e.g. communication, training, inspections and audits)
- More communication and training = higher levels of voluntary compliance
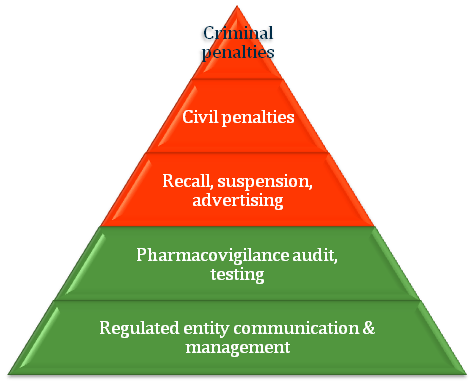
Achieving compliance can be viewed as a pyramid. As with any pyramid, if the base is not sound, the structure will fail; getting the base of the pyramid right is a fundamental success factor. Thus, communication (the base of the pyramid) and identification of the level of compliance for different regulated entities (the second level of the pyramid) are key components to the successful regulation of compliance.
Managing compliance risks
If realised, risks related to the compliance of regulated entities may impact on the health and wellbeing of Australian consumers of therapeutic goods. It is therefore important for TGA to manage these risks.
The attitude of the TGA to the regulated entities depends on the compliance risk, i.e. how likely the entity is to fail (accidentally or deliberately) to comply with legal requirements. Compliance risks need to be identified, with different risks managed in different ways. The TGA aims to help, support, inform and advise those who are trying to be compliant. Those who do not wish to comply need to be deterred by detection, and if necessary, enforcement action.
The detection of compliance issues is assisted by the testing laboratories at the TGA, which conduct both random and targeted testing of products that are marketed in Australia. Once a compliance issue has been detected, the TGA can work with the regulated entity to try to help the entity comply. If non-compliance continues, then, when appropriate, TGA investigators can prepare a brief of evidence that is then referred to the Commonwealth Director of Public Prosecutions.
For more information, see Compliance management.
| TGA compliance strategy | |||
|---|---|---|---|
| Help and support | Inform and advise | Correct behaviour | Enforcement action |
| Make ongoing compliance easy | Help to become and stay compliant | Deter by detection | |
| Regulated entity - attitude to compliance | |||
| Voluntary compliance | Accidental non-compliance | Opportunistic non-compliance | Intentional non-compliance |
|
|
|
|
| "Committed to doing the right thing" | "Trying to do the right thing but don't always succeed" | "Don't want to comply but will if made to" | "Decision to not comply" |
   | |||
TGA as a world-class regulator
TGA has invested significant effort into establishing itself as a leading regulator of therapeutic goods. This has involved:
- attracting staff with the right balance of technical and regulatory skills
- supplementing this world-class expertise with external experts (TGA advisory committees)
- working closely with international regulators
- developing appropriate regulatory processes
- developing timely and appropriate internal and external communication processes
The effective management of both product risks and compliance risks depends on the collection, collation and analysis of information from all regulatory areas of TGA.
Applying a collaborative, whole-of-regulatory-cycle view of therapeutic goods and regulated entities allows TGA to tailor appropriate risk management strategies.
Effective communication and collaboration between different areas of the TGA are facilitated by the following:
- TGA being structured along functional responsibilities
- identification of the existing interdependencies between TGA regulatory areas in order to facilitate collaboration
- lines of communication and collaboration that maximise the ability to identify and manage product safety risks and regulated entity compliance risks
- the implementation of processes to improve how the TGA communicates and provides information to stakeholders
In summary, the key features of the TGA regulatory framework are:
- a risk-based approach is taken to regulation, with different levels of risks for different products
- regulation occurs both pre-market and post-market
- both product risks and compliance risks are regulated
- there is a focus on fostering voluntary compliance among the TGA regulated community
- continual improvement is achieved by ongoing review and changes to the regulatory structures and processes

